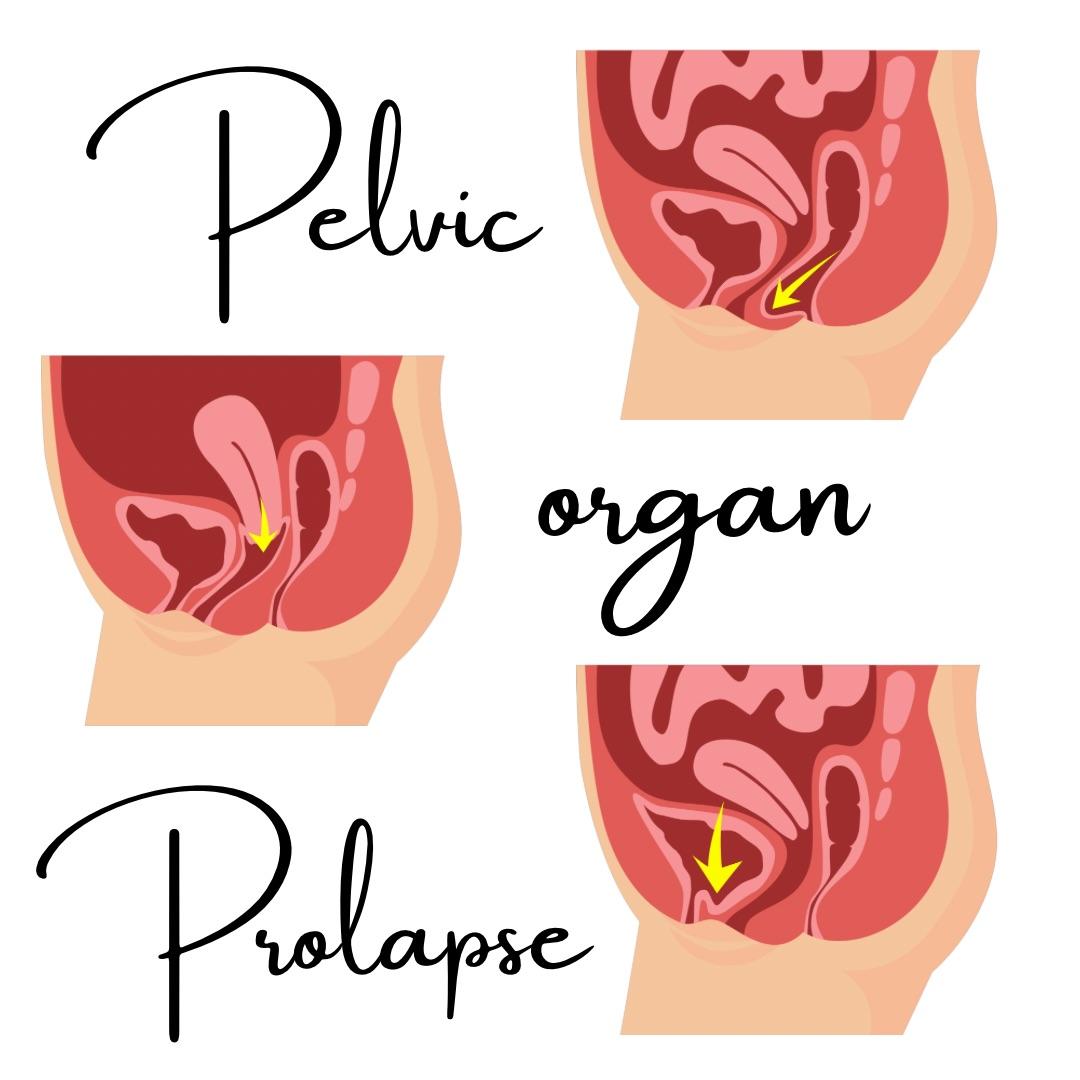
C-Section Recovery: The Healing No One Prepared You For
In honor of C-Section Awareness Month
You had major abdominal surgery…and then were handed a newborn.
No roadmap.
No real recovery plan.
No one explaining what your body just went through.
So you did what most moms do—you powered through.
You lifted the baby.
You managed the house.
You ignored the pulling, burning, numbness, or pressure…because life didn’t slow down, even if your body needed it to.
But here’s the truth:
C-section recovery isn’t just about the incision healing.
It’s about how your entire body adapts, compensates, and (hopefully) recovers after surgery.
What Actually Happens During a C-Section
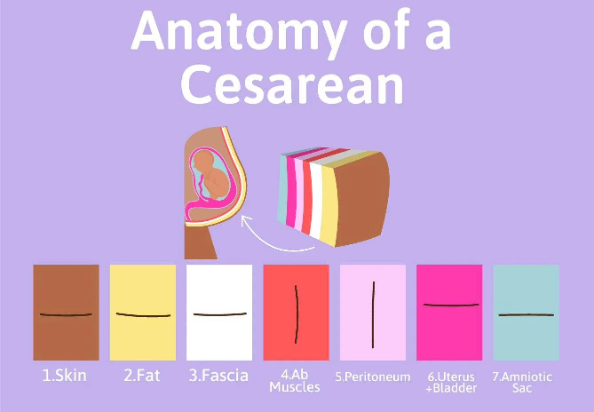
A cesarean birth involves multiple layers:
- Skin
- Fat/Adipose tissue
- Fascia
- Abdominal muscles (which are separated, not cut—but still affected)
- Peritoneum (membrane lining abdominal cavity)
- Uterus
- Bladder (pulled out of the way)
- Amniotic Sac
Each of these layers heals at a different rate. And more importantly—they don’t always heal well together without guidance.
This is where issues can begin.
Common Symptoms Moms Experience (But Are Told Are “Normal”)
- Tightness or pulling around the scar
- Numbness or hypersensitivity
- A “shelf” or bulging above the incision
- Core weakness or doming
- Low back or hip pain
- Pain with movement, exercise, or even laughing
- Feeling disconnected from your core
These are common—but they are not something you just have to live with.
Why Your Scar Matters More Than You Think
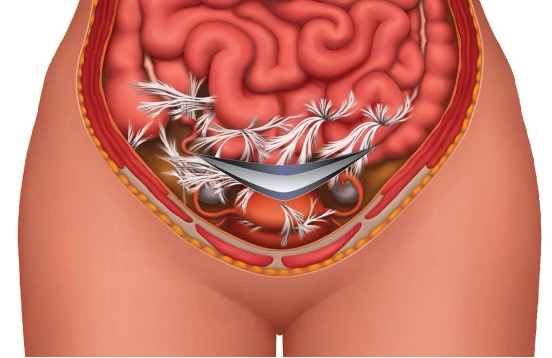
Your scar is not just a line on your skin.
It can create adhesions—areas where tissue sticks together instead of gliding smoothly.
That matters because your body works as a system:
- Your diaphragm
- Your core
- Your pelvic floor
If one area is restricted (like your scar), everything else has to compensate. That’s when you start seeing:
- Leaks
- Pressure
- Pain
- Weakness
The Missing Piece: Retraining, Not Just Resting
Most moms are told: “Don’t lift anything heavier than your baby.”
…and then eventually: “You’re cleared—go back to normal.”
But there’s a huge gap in between.
Healing should include:
- Restoring mobility in the scar and surrounding tissue
- Reconnecting to your deep core system
- Retraining pressure management (so you’re not bearing down with daily movements)
- Gradually rebuilding strength in a way that supports—not strains—your body
This is exactly where pelvic floor physical therapy comes in.
What Recovery Should Feel Like
With the right guidance, you can:
- Move without pulling or pain
- Feel strong and connected through your core
- Lift your kids (and weights) confidently
- Reduce or eliminate that “shelf” appearance
- Return to workouts safely
- Actually feel like yourself again
You Don’t Have to “Just Live With It”
C-section recovery is often minimized—but it shouldn’t be.
You deserve:
- A plan
- Support
- Real healing—not just time passing
And the best part?
It’s never too late to start.
Even if you’re months—or years—postpartum.